Spinal Conditions: Sciatica and Leg Pain
The term “sciatica” refers to pain that is felt down the leg. The sciatic nerve is the large nerve that runs down the back of your leg. It is made up of several spinal nerves. Spinal surgeons tend to use the term radiculopathy or radicular pain rather than sciatica because it is usually a spinal nerve and not the sciatic nerve that is causing the pain.
Leg pain arising from the spine is usually due to spinal nerve compression and it is often felt going down the whole leg. Many patients with degenerative low back pain can experience leg pain, which is typically far less severe than the back pain, and it rarely goes below the knee. In contrast, patients with spinal nerve compression usually have far more leg pain than back pain.
Compression of a spinal nerve will usually cause symptoms of leg pain, numbness and tingling. Sometimes part of the leg can become weak and rarely bladder and bowel dysfunction can occur. The leg pain is usually severe and sharp. It is often described as burning in nature or like an electric shock.
Of course leg pain can have many different other causes. It can be classified into pain of spinal origin and non-spinal origin. For example, a disc herniation and spinal stenosis are spinal causes of leg pain, whereas osteoarthritis of the hip and knee are non-spinal causes of leg pain.
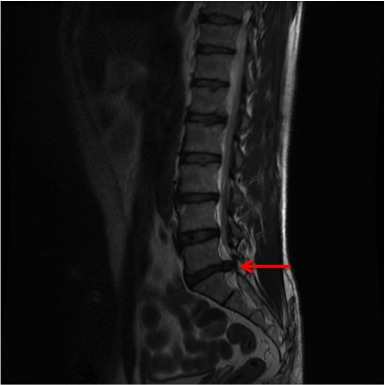
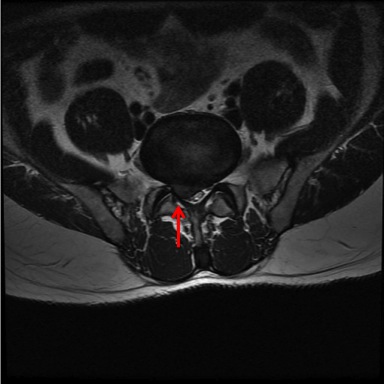
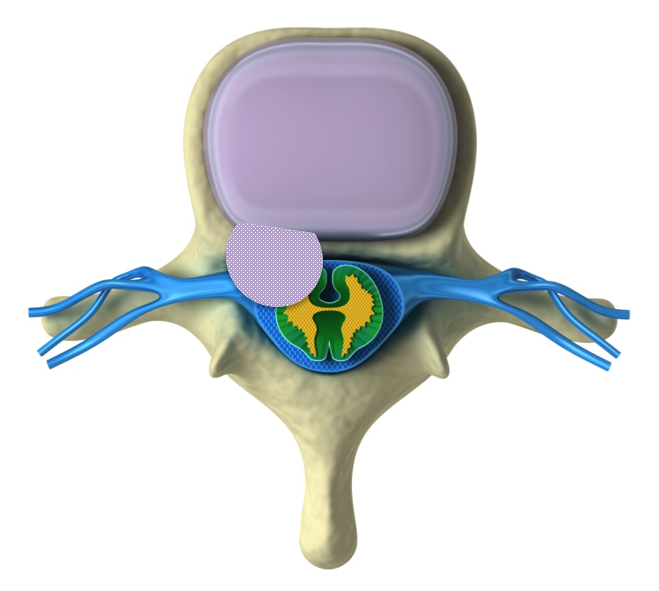
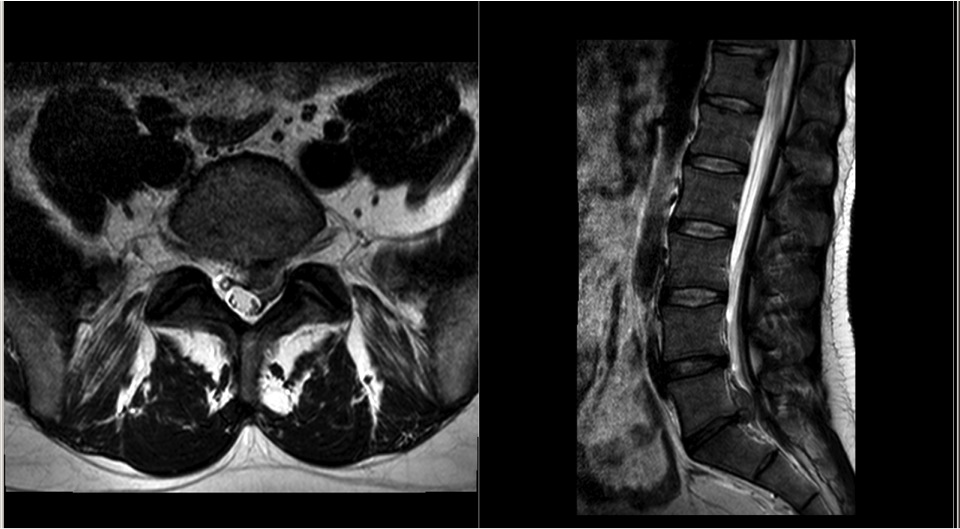
Disc Herniation / Prolapse
Disc herniation, frequently known as a disc prolapse or slipped disc, is very common. Around 1% - 2% of the population will have an episode of leg pain lasting more than two weeks as a result of a disc herniation. It most frequently occurs in adults between thirty and fifty years of age. As the intervertebral disc undergoes the normal aging process, the stiff outer fibrous layer can crack and a small volume of the central jelly like disc material can escape through the defect. When this occurs, the disc material can cause inflammation and can press on the spinal nerves in the spinal canal. The inflammation that occurs is part of the body’s normal healing response. Both the mechanical compression of the nerve root and the inflammation around it can act to irritate the nerve resulting in leg pain, numbness and weakness.
95% percent of lumbar disc herniations occur at L4 / 5 and L5 / S1 levels and most leg pain improves or resolves without any medical intervention. By six weeks 60 to 80% of patients have improved, rising to 90% by twelve weeks. Serial spinal imaging studies have shown that up to 80% of disc herniations reduce in size by over 50% with the passage of time. This is due to the body’s own healing mechanisms. It has been shown that static mild weakness in the leg (that does not worsen) resolves equally as well with conservative management versus surgical intervention.
Surgery for a disc herniation is indicated in the following situations:
- Cauda Equina Syndrome (see below)
- Neurological deterioration – this usually means worsening of any weakness in the leg
- Failure to improve with conservative management with persistent leg pain
The factors that are associated with good surgical outcomes are:
- Leg pain worse than back pain
- Neurological symptoms are consistent with nerve root irritation
- Neurological examination is consistent with nerve root irritation
- Nerve root tension signs are positive on clinical examination
- Investigations are consistent with the patients symptoms and clinical examination (i.e. MRI scan)
- Pain longer than six weeks
Surgery versus conservative management:
It is important to understand that surgery for a disc herniation, which is causing leg pain, carries with it risks. Various clinical studies have shown that there is no difference in the clinical outcomes of patients treated operatively versus those treated non-operatively after four to ten years. The Microdiscectomy procedure has been shown to offer better outcomes than conservative treatment at the one-year mark but by two years there was no difference between patients treated surgically and those treated non-surgically. It appears that both patients treated surgically and non-surgically show substantial improvement in all outcome measures over two years but there is a tendency for the results to favour the surgical group (although this was not significant in statistical terms). In a large study of patients followed up for ten years, up to 25% (one in four) of those treated surgically went on to have an additional operation and up to 25% (one in four) of those treated non-surgically went on to have an operation because of persistent symptoms. It has been shown that earlier surgery for persistent leg symptoms due to a disc herniation of less than one-year duration appears to offer a better outcome. It is thought that beyond this time chronic pain can develop and this pain persists despite technically successful surgery.
Overall, surgery for a disc herniation can be up to 80 to 90% successful in providing significant improvement in leg pain. However, one in ten patients may not notice any improvement and up to one in twenty patients may develop chronic pain due to nerve scarring. The recurrence rate for a subsequent disc herniation is around 10% over ten years either at the same spinal level or at a different one. The incidence of back pain post discectomy ranges from 10 to 30% and is related to the amount of disc material removed. Interestingly, spinal fusion for post discectomy low back pain, in the absence of degenerative changes at other levels of the spine, seems to have a more favourable outcome than spinal fusion for degenerative disc disease.
Disc Herniation / Prolapse Causing Low Back Pain
Disc herniations are often associated with low back pain but this pain is likely to be due to the underlying degenerative disc disease rather than the herniation / prolapse itself. Discectomy procedures for low back pain have generally been discontinued in modern day spinal surgery. As mentioned in the low back pain section, surgery for back pain is unpredictable. Surgery for leg pain however is far more predictable. By taking the pressure off a compressed nerve the leg pain tends to improve. The same is unfortunately not true for back pain.
Cauda Equina Syndrome
Cauda equina syndrome is a very rare but serious condition. It consists of a combination of low back pain, pain in one or both legs, numbness and / or weakness in the legs, numbness in the genitals and / or bottom region and urinary and / or rectal symptoms (such as incontinence and the inability to pass urine). All of these symptoms can have varying degrees of severity. The incidence is approximately 2 in 1,000,000 of the population. It is considered to be a surgical emergency that requires urgent intervention to prevent permanent loss of bladder and bowel function. It is usually due to a massive disc prolapse that compresses all of the nerves in the spinal canal. It is normally of sudden, unexpected onset. It uncommonly occurs in patients with known disc prolapses as seen on MRI scans (unless they are very large prolapses) and it occurs only rarely in patients with spinal stenosis.
It is felt that the outcome of cauda equina syndrome is related to the time taken to get to the operating theatre and undergo decompressive surgery (i.e. the sooner the better). But, as with all things in life it is often more complicated than that. Overall, 75% of patients will have acceptable urinary function following cauda equina syndrome. Unfortunately, up to 20% will have poor outcome.
Spinal Stenosis
Spinal stenosis is a condition in which there is narrowing of the spinal canal and, therefore, a reduction in space for the nerves. It is usually due to degenerative changes in the spine that have occurred over many years. The intervertebral disc can be thought of as a car tyre - over time it deflates and bulges. As this occurs the height is lost at the front of the spine and the facet joints at the back of the spine start to take more load. Facet joint degeneration then occurs and the joints and ligaments can enlarge. The ligaments at the back of the spine tend to buckle inward as the disc height is reduced and they become lax. Narrowing of the spinal canal and space for the nerves then occurs due to a combination of the disc bulge, facet enlargement (hypertrophy) and ligament buckling (ligamentum flavum hypertrophy).
Spinal stenosis typically gives leg symptoms due to nerve compression and this is discussed further in the spinal stenosis and spondylolisthesis section. The back pain symptoms are generally due to the degenerative changes that have taken place and their management is discussed in the low back pain section. Occasionally when decompressive surgery is performed for leg symptoms in patients with spinal stenosis the back pain can improve but this is unpredictable. Surgery for back pain alone in spinal stenosis is rarely performed.
Not infrequently the degenerative process described above can result in a spondylolisthesis. This is when one vertebra slips forward on the other. This is called a degenerative spondylolisthesis. The spinal canal can become markedly narrowed and nerve symptoms in the legs can occur from compression in the narrowed spinal canal and narrowed neural foramens (the place where the nerves exit the spine). Spondylolisthesis can also occur when there is a spondylolysis and subsequent disc degeneration (a spondylolytic spondylolisthesis). There are also many other causes of a spondylolisthesis. This is discussed further in the spinal stensosis and spondylolisthesis section.
Spinal Tumours, Infections, Trauma and Deformity (Scoliosis and Kyphosis)
These conditions can cause leg pain if compression of a nerve root occurs. The treatment varies and is aimed at the underlying cause.
Nerve Root Blocks
Nerve root blocks can be a simple and low risk way of alleviating nerve root pain due to disc herniation or stenosis. They can effectively reduce pain by up to 60 to 80%. In patients who are considered to be good surgical candidates, 50 to 60% will have an improvement in their pain such that they subsequently avoid an operation. More information on Nerve Root Blocks can be found in one of my patient information leaflets.
Non-Spinal Causes of Leg Pain
The following conditions can also cause leg pain:
- Vascular pathology (problems with the blood supply to the leg)
- Neuropathy (problems with the small nerves in the leg)
- Sacroiliac joint pain
- Hip pathology - osteoarthritis, trochanteric bursitis (pain and inflammation around the outer aspect of the hip), hamstring injury
- Knee pathology - osteoarthitis, meniscal / cartilage tears, calf injury, deep venous thrombosis (clots in the calf)
- Foot pathology – osteoarthritis, gout, metatarsalgia (pain in the bones and joints of the toes), plantar fasciitis (pain in the sole of the foot)
Further Information on Sciatica and Leg Pain
More information on sciatica and leg pain can be found in the following documents and in the Useful Links section of this site. Please note that some of these documents are written for health care professionals.
Information on disc prolapse from Patient.co.uk
Patient information from the North American Spine Society
Leg Pain Option Grid: this can help make choices for those suffering from this condition
Dr Mike Evans has an introductory video for low back pain: